Treating bacterial infections without antibiotics might sound like a problem from another time, but it is a challenge that healthcare professionals in remote areas are facing.
Antibiotic shortages are transforming ‘school sores’ (impetigo), a treatable bacterial skin infection common amongst Indigenous children in remote areas, into a far more complex health-threat.
According to Sam Keitaanpaa, a Clinical Service Specialist Pharmacist in the Northern Territory specialising in vulnerable groups, school sores – the colloquial name for impetigo due to its common occurrence amongst young school children – is usually caused by Staphylococcus or Streptococcus bacteria. It is highly contagious and easily transmitted through contact with the fluid or crusts of an impetigo sore.
He said that school sores are particularly prevalent amongst Aboriginal and Torres Strait Islander children in remote areas due to overcrowding in households, as well as existing issues around hygiene and access to health care.
Even so, he noted that they are usually a ‘minor inconvenience’ and can be treated with simple wound care, occlusion to prevent transmission and benzathine benzylpenicillin or trimethoprim-sulfamethoxazole if necessary.
Mr Keitaanpaa said that in remote areas, benzathine benzylpenicillin is often preferred as it doesn’t require ongoing oral antibiotic therapy. However, it can only be administered via injection, and therefore requires access to a GP.
As an alternative, trimethoprim-sulfamethoxazole is prescribed. Unlike benzathine benzylpenicillin, it is available as a tablet or suspension. The suspension is preferable for children but is currently in short supply.
Asha Bowen, a clinician researcher working at Perth Children’s Hospital as a Paediatric Infectious Diseases Specialist, recently noted in The Conversation that the medicine was previously available under the brand names Bactrim and Septrin. But, in September 2018, Bactrim was removed from the market – placing extreme pressure on Septrin manufacturers to meet the needs of children around the country. As a result, per TGA, there is currently limited availability of Septrin liquid, Resprim and Resprim Forte tablets, while Septrim Forte tablets are for emergency supply only.
‘What is often not understood by patients is that there is not one machine putting out one medicine. Rather, they are manufactured in batches and these are planned in advance in order to produce a range of medicines,’ Mr Keitaanpaa said. ‘When this is disrupted, it can take a while to rectify and get more product to market.’
The difficulty in accessing the required antibiotics means cases of impetigo can quickly become more severe. Mr Keitaanpaa said that it has been linked to post-streptococcal glomerulonephritis, which can lead to irreparable kidney damage. This is particularly concerning, given the additional risk factors for kidney disease amongst Aboriginal and Torres Strait Islander people. Mr Keitaanpaa noted that damage in young people can pose a risk of morbidity.
In addition to kidney disease, A/Prof Bowen noted that untreated sores can also lead to rheumatic fever, bone infections or sepsis. This can play a part in perpetuating further inequality in remote Indigenous communities – with children taking time out of school to avoid further transmission and, potentially, cope with long-term, chronic illnesses.
Treatment options
While the absence of antibiotics makes treatment challenging, pharmacists can play a valuable role in controlling the infection until medicine becomes available.
The first priority in managing school sores in a pharmacy environment is proper wound care and occlusion, Mr Keitaanpaa said.
‘The skin should be washed with soap or an antiseptic wash and then covered with a crepe bandage or a suitable wound dressing. This both promotes proper wound healing and clearing of the infection as well as reducing the risk of transmission to other people the person may come in to contact with.’
He also urged pharmacists to inform patients and their carers of the signs of more serious infections, such as poor wound healing and increasing signs of malaise.
Meanwhile, since January it has been mandatory for manufacturers to report drug shortages to the Therapeutic Good Administration so that healthcare practitioners and their patients can be informed of supply problems in advance.
While this policy may help patients and healthcare practitioners in the future, A/Prof Bowen said that the need to ensure healthy supplies of the medicine is pressing.
‘With 15,000 Aboriginal children at any one time needing this antibiotic to treat school sores, the demand is real,’ she said.
Hear about pharmacists working to close the gap in with Aboriginal health services at the PSA19 conference in Sydney from 26–28 July. Register now to attend.




 This CPD activity is sponsored by Reckitt. All content is the true, accurate and independent opinion of the speakers and the views expressed are entirely their own.[/caption]
This CPD activity is sponsored by Reckitt. All content is the true, accurate and independent opinion of the speakers and the views expressed are entirely their own.[/caption]
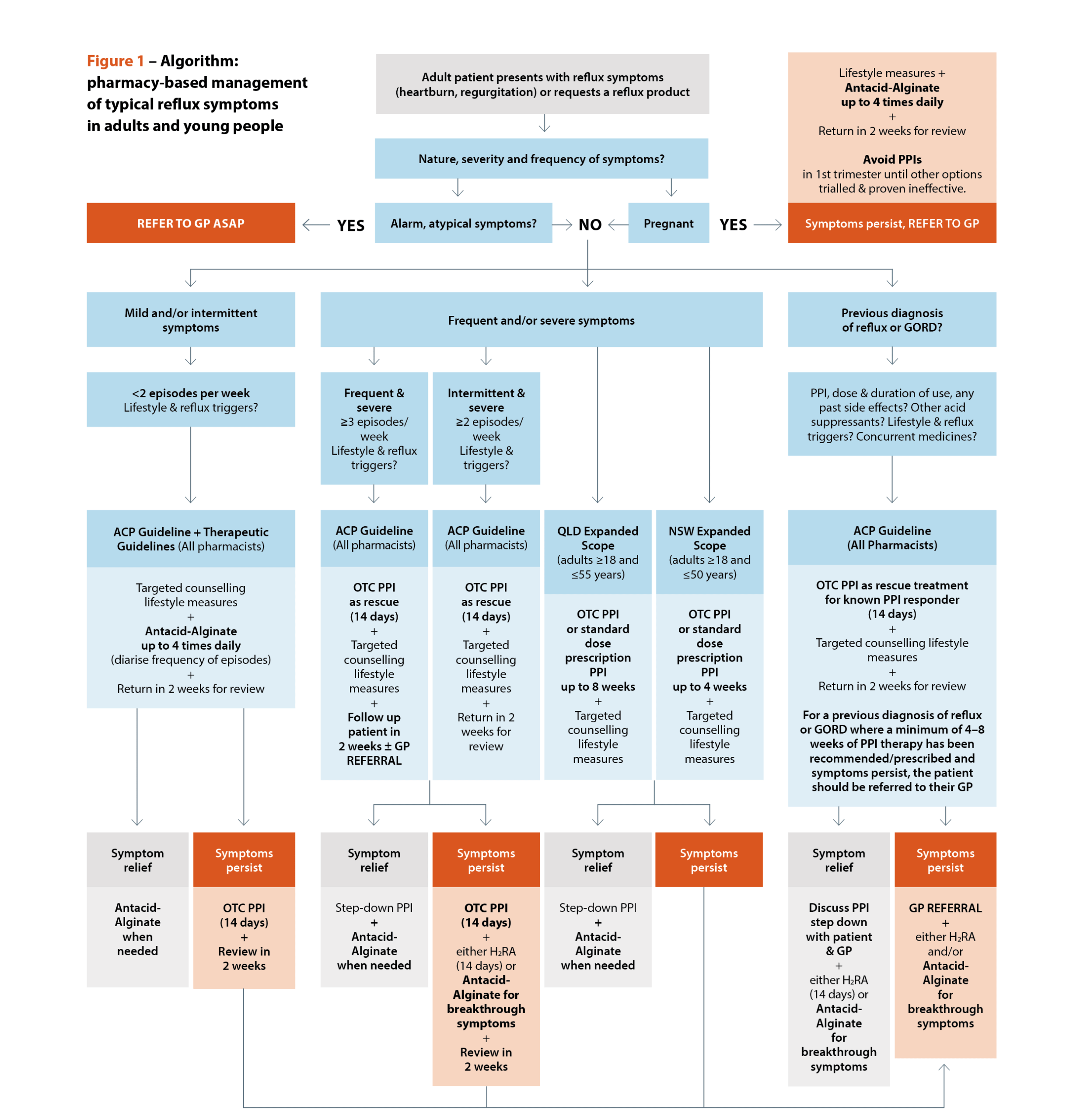 Sources: Australasian College of Pharmacy. Management of reflux: a guideline for pharmacists. Queensland Health. Queensland Community Pharmacy Gastro-oesophageal Reflux and Gastro-oesophageal Reflux Disease – Clinical Practice Guideline. NSW Health. NSW Pharmacist Practice Standards for gastro-oesophageal reflux and gastro-oesophageal reflux disease.[/caption]
Sources: Australasian College of Pharmacy. Management of reflux: a guideline for pharmacists. Queensland Health. Queensland Community Pharmacy Gastro-oesophageal Reflux and Gastro-oesophageal Reflux Disease – Clinical Practice Guideline. NSW Health. NSW Pharmacist Practice Standards for gastro-oesophageal reflux and gastro-oesophageal reflux disease.[/caption]

 Dr Ming S Soh PhD, BPharm (Hons)[/caption]
Dr Ming S Soh PhD, BPharm (Hons)[/caption]






 DR Amy Page (she/her) PhD, MClinPharm, GradDipBiostat, GCertHProfEd, GAICD, GStat, FSHPA, FPS is a consultant pharmacist, biostatistician, and the director of the Centre for Optimisation of Medicines at UWA’s School of Allied Health.[/caption]
DR Amy Page (she/her) PhD, MClinPharm, GradDipBiostat, GCertHProfEd, GAICD, GStat, FSHPA, FPS is a consultant pharmacist, biostatistician, and the director of the Centre for Optimisation of Medicines at UWA’s School of Allied Health.[/caption]

 Hui Wen Quek (she/her) BPharm(Hons), GradCertAppPharmPrac is a pharmacist and PhD candidate at the University of Western Australia (UWA).[/caption]
Hui Wen Quek (she/her) BPharm(Hons), GradCertAppPharmPrac is a pharmacist and PhD candidate at the University of Western Australia (UWA).[/caption]







