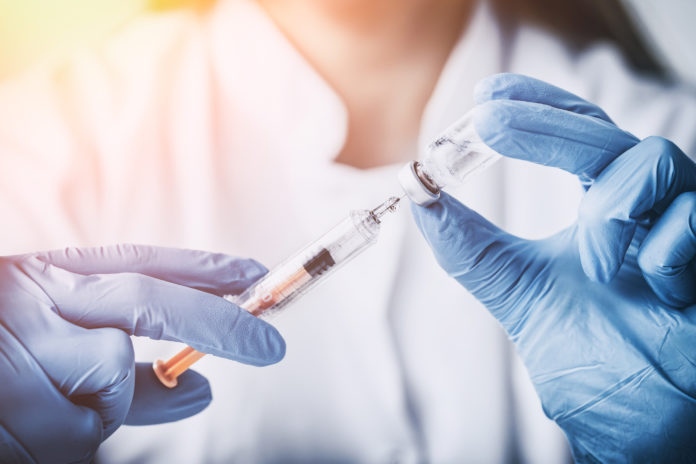
Australia’s first pharmacist-administered vaccine trial began in 2014. Since then, pharmacist immunisation programs have begun in every state, and are now essential to public and preventative health in Australia. And there could be more to come.
It’s only two years since all Australian states and territories began allowing pharmacists to administer vaccines in the community but in that time such services have grown dramatically.
In 2015, the second stage of Queensland’s QPIP trial saw 22,835 influenza, 1,834 pertussis and 33 measles vaccinations administered.1 By September of the following year, the Chemist Warehouse chain of pharmacies alone had administered 200,000 vaccines nationally.2
In Victoria, approximately 270 pharmacies are registered with the Department of Health and Human Services (DHHS) to provide vaccination services in the community.3 In South Australia, more than 260 pharmacies – 54% of the state total – are registered to provide vaccination services.4 Pharmacist-administered vaccinations are now commonplace, and will play an increasingly important role in Australia’s health system. Up to October 2017, 6,790 pharmacists have completed PSA training courses, and over 400 are currently enrolled, according to PSA National Training Manager Dorothy Lucardie.
Fractured framework
While increasing numbers of Australians are easily accessing a range of vaccinations at their local community pharmacy, the legislative framework governing the service is complex and fractured.
‘It’s very fluid in practice. We have eight jurisdictions, each with different legislation,’ said Denise Hope, pharmacist and lecturer at Griffith University School of Pharmacy and Pharmacology. While Queensland, New South Wales and the Australian Capital Territory allow interns to administer vaccines under supervision from a qualified pharmacist, the remaining states do not. Likewise, Victoria, South Australia and Tasmania require pharmacies to register with the state health department to provide vaccination services, while the remaining states require no additional registration.
All states require pharmacists to be up to date with first aid, CPR and anaphylaxis management, but the certification requirements for these competencies vary between states. NSW, Western Australia and Tasmania only allow qualified pharmacists to administer influenza vaccinations, while the remaining states have expanded the service to include diphtheria, tetanus and pertussis (dTpa) vaccines and in some cases the measles, mumps and rubella (MMR) vaccine. South Australia allows diphtheria, tetanus and pertussis with inactivated polio vaccine dTpa-IPV.
PSA in each state provides state-specific information, and can also provide information for pharmacists moving between different jurisdictions.
Missing the herd
‘Really, this is about increased access. We’re giving another opportunity for people to get immunised, increasing the chance of Australia reaching herd immunity,’ said Chris Campbell, the PSA Vice President for Queensland.
Studies have estimated the vaccination coverage required to establish herd immunity against influenza viruses at 80-90%.5 Australia’s vaccination rate ranges from 27% across the population to 74% for at-risk groups such as Australians aged 65 years and over.6,7
Pharmacist-administered vaccines play an important role in increasing Australia’s vaccination rate. The QPIP study revealed that up to 17% of participants would not have had the influenza vaccine if the pharmacist-administered service was not available.
A 2017 study found two million Australians who weren’t considering getting the influenza vaccine would do so if they could get it at a pharmacy.
‘Access helps with vaccines and herd immunity, especially in terms of being able to simply go and get them at a pharmacist, no appointment necessary,’ said Mr Campbell.
Improving vaccination rates doesn’t just apply to influenza. While Australia has a strong childhood vaccination program, there are many areas in Australia with vaccination rates still below the level of coverage required for herd immunity, including for dTpa and MMR.
In recent years, there have been multiple outbreaks of pertussis, with dramatic increases in notified cases in NSW and South Australia.
‘I think we’ve forgotten the catastrophic effect some of those viral-borne diseases have had on our community in the past. I think it’s been lost off our radar,’ said Helen Stone, PSA Branch Director for South Australia and in Northern Territory.
Ease of access
Providing vaccination services at a pharmacy, many of which are open outside of work hours, during weekends, and even 24 hours, not only means vaccines are more accessible, but can also drive efficiency in the healthcare system. ‘Traditionally if a patient went to their GP for an influenza or whooping cough vaccine they would have been written a script which they would then need to go to the pharmacy to have dispensed, then they would have to take it back to the clinic where they would then have the doctor or nurse administer it,’ said Anthony Harris, Pharmacist at Priceline Pharmacy in Woden, ACT.
Victoria is the only state that allows pharmacists to administer vaccines to high-risk groups under the National Immunisation Program (NIP). In all other states, the vaccinations come at a net zero cost to the government, reducing the burden on the Medicare budget.
Patients don’t have to pay a consultation fee, and there’s no waiting time, but Mr Campbell said there are benefits for GPs. ‘We have pharmacies that are co-located with a GP practice, and we’re getting referrals both ways; from the GP to the pharmacy for immunisations, and from the pharmacy to the GP for the NIP-qualified,’ he said.
The experience of many pharmacists is that pharmacy-based vaccinations have been well received by the community. ‘They’ve got no problem with a pharmacist vaccinating them, because in reality, in a GP practice it’s rarely the GP that gives the needle anyway,’ said Karalyn Huxhagen, a rural consultant pharmacist working in Mackay, Queensland.
Ms Huxhagen said the majority of the vaccinations she administered were influenza and dTpa. While the Mackay pharmacy offers an online booking service, the majority of their vaccinations come from walk-in patients.
A rural solution
‘In metropolitan areas I think we take for granted how quickly we can access a GP. If you start going out into rural or remote areas, patients may have waits of weeks on end to even see a GP,’ said Griffith University’s Ms Hope.
Providing essential health services, including vaccinations, in rural and remote Australia has long been a challenge for Australia. Allowing pharmacists to prescribe medications in rural areas had previously been suggested by the National Rural Health Alliance as a way to improve the health of Australians disadvantage by remoteness.
Opening up vaccination services to community pharmacists has meant improved access to these services in towns that have a pharmacy, but no permanent doctor.
‘In a lot of our rural and remote towns in South Australia, in particular, the pharmacist is often the only health professional who is consistently in those communities,’ Ms Stone said. Of South Australia’s 261 pharmacies registered to provide vaccinations, 88 are registered for extended services, such as dTpa, dTpa-IPV and MMR, and 22 of these are in rural or remote locations. Rather than travelling considerable distances to get vaccinated, or worse, simply neglecting to get vaccinated at all, more Australians living remotely can now access these services through a local pharmacy.
Where to next
Pharmacist-administered vaccines are now an important part of public health and preventative medicine in Australia, even providing these essential services in places where they weren’t previously available. There is the potential to add to the list of approved vaccines.
Ms Stone said she believed that pharmacists should have wider access to the NIP. ‘Considering our training, it’s appropriate that pharmacists should be able to access the NIP, especially in a pandemic to contribute to the public health response. Give pharmacists access under the NIP, and let’s just vaccinate everyone for flu,’ Ms Stone said.
There have also been calls for aligning regulation on age limits for pharmacist vaccines with age guidelines for pharmaceuticals generally. ‘Our definition of an adult being anyone 18 and over is not appropriate, especially in the immunisation and medication space where we will treat people aged 12 and up as an adult in terms of medication and dose,’ Mr Campbell said. ‘If the regulation allowed for 12 years and up, we’d automatically start to reach the teenage, high-school population.’
Ultimately, Ms Stone said the regulation around pharmacist-administered vaccines urgently needs to change. ‘We need consistency across the country,’ said Ms Stone. ‘The evidence shows that having a vaccine administered in a pharmacy is as safe as having it administered in any other setting. Regardless of which state or territory they’re in, pharmacists can vaccinate people safely, and the legislation should be the same right across the country.’
(This information is accurate as of 19 February 2018.)
Regulations for Pharmacist-administered vaccinations
While regulation governing pharmacist-administered vaccinations changes from state, all states require pharmacists to complete vaccination training with a recognised training provider, such as PSA.
Only pharmacists working in Tasmania need to register as a pharmacist immuniser with the Tasmanian Department of Health and Human Services. Pharmacies in Victoria, South Australia and Tasmania need to register with the state’s health department.
Pharmacists also need to have a current First Aid and CPR certificate, as well as training to handle anaphylaxis, which can be completed online with the Australian Society for Clinical Immunology and Allergy (ASCIA). Only Queensland, NSW and the ACT allow interns to vaccinate under supervision.
Beyond the training and registration requirements, the premise and equipment requirements vary little from state to state: a private, uncluttered, designated vaccination area with appropriate lighting, hand sanitation facilities, and space for two staff to work and for the patient to lie down if necessary.
Karalyn Huxhagen, a pharmacist in Mackay, Queensland, said setting up an appropriate space was simple. ‘We already had a counselling room, as we provide professional services,’ she said. ‘It was a no brainer to have EpiPens, gloves, hand sanitiser and other equipment that we already had because we do cholesterol and BP checks.’
Similarly, the majority of pharmacies will already have the refrigeration facilities required to maintain vaccine cold chain.
‘It wasn’t hard,’ said Ms Huxhagen. ‘The cost of the immunisation up-scaling wasn’t major. The PSA ran road shows and we availed ourselves of that, and we already keep our first aid qualifications up-to-date because as pharmacists I think that’s something we need to do.’
Adequate indemnity insurance is also a standard requirement under state regulation and the Pharmacy Board of Australia registration standard, and cover for vaccination services is now included under standard policies. ‘Immunisation and administering of medications is now within a pharmacist’s scope of practice, so that’s covered by a current indemnity. So, no extreme indemnity is needed for a pharmacist that immunises,’ said Chris Campbell, PSA Vice President for Queensland.
State by State Regulations17-24
| QLD | |
| Who can vaccinate? | Pharmacist, Intern under supervision |
| Vaccines authorised | Influenza, dTpa, MMR |
| Age of patient | 18+ |
| VIC | |
| Who can vaccinate? | Pharmacist |
| Vaccines authorised | Influenza, DTP, dTpa |
| Age of patient | 18+ |
| TAS | |
| Who can vaccinate? | Pharmacist |
| Vaccines authorised | Influenza |
| Age of patient | 18+ |
| SA | |
| Who can vaccinate? | Pharmacist |
| Vaccines authorised | Influenza, dTpa and dTpa-IPV, MMR |
| Age of patient | 16+ |
| NT | |
| Who can vaccinate? | Pharmacist |
| Vaccines authorised | Influenza, DTP, MMR, dTpa |
| Age of patient | 16+ |
| WA | |
| Who can vaccinate? | Pharmacist |
| Vaccines authorised | Influenza |
| Age of patient | 18+ |
| NSW | |
| Who can vaccinate? | Pharmacist, Internvunder supervision |
| Vaccines authorised | Influenza |
| Age of patient | 18+ |
(This information is accurate as of 19 February 2018.)
PSA immunisation courses
The PSA offers multiple courses each month to support pharmacists in their professional development and provision of vaccination services.
PSA’s Pharmacist Immunisation Training Program consists of online prerequisite learning modules and a one-day face-to-face workshop. The program is APC approved and recognised by each jurisdiction.
Immunisation training is $550 for members and $640 for non-members, and includes online modules, a day of face-to face training, and administering practice vaccines of normal saline.
‘PSA used immunisers who do a lot of workplace immunisation programs to do the training, so they are really very good,’ said Karalyn Huxhagen, a pharmacist in Mackay, Queensland.
PSA provides support to immunisers with short refresher workshops, guidelines, immunisation-related CPD and transition information to support pharmacists to change jurisdictions or understand an expansion to the scope of immunisations.
PSA members can access all of these resources via the dedicated PSA Immunisation Resource Hub at www.psa.org.au/immunisation
References
- Pharmaceutical Society of Australia. Vaccinations in Pharmacy. 2016. At: http://www.mvec.vic.edu.au/wp-content/uploads/2016/12/CVU-2016_Vaccinations-in-Pharmacy-by-Emma-Abate.pdf
- Department of Health. Review of Pharmacy Remuneration and Regulation Submission #218. 2016. At: https://www1.health.gov.au/internet/main/publishing.nsf/Content/review-pharmacy-remuneration-regulation
- Pharmacist-administered vaccination services. 2018. At: https://www2.health.vic.gov.au/public-health/immunisation/immunisers-in-victoria/pharmacist-immunisers/vaccination-services
- SA Health. Approved organisations – Pharmacies. 2018. At: http://www.sahealth.sa.gov.au/wps/wcm/connect/908e91004288ecd5a2b3ba80c298878e/2018_01_31%2BApproved%2BPharmacies.pdf?MOD=AJPERES&CACHE=NONE&CONTENTCACHE=NONE
- Plans-Rubió P, The vaccination coverage required to establish herd immunity against influenza viruses. Preventative Medicine 2012; 55, 1; 72-77
- Sullivan SG, Chilver MB, Carville KS, et al. Low interim influenza vaccine effectiveness, Australia, 1 May to 24 September 2017. Eurosurveillance 2017; 22, 43.
- Australian Institute of Health and Welfare, 2009 Adult Vaccination Survey: summary results. 2011. At: https://www.aihw.gov.au/reports/primary-health-care/2009-adult-vaccination-survey-summary-results/contents/table-of-contents
- Diphtheria death shows Queensland is failing to properly vaccinate, AMA warns. 2018. http://www.abc.net.au/news/2018-02-08/diptheria-deathshows- vaccination-failure-ama-says/9407920
- vic. Victorian Pharmacist-Administered Vaccination Program Guidelines. 2016. At: https://www2.health.vic.gov.au/~/media/health/files/collections/policies%20and%20guidelines/v/victorian-pharmacist-administeredvaccination-guidelines%20-%20pdf.pdf
- Pharmacy Guild of Australia. Queensland pharmacist vaccination standard. 2016. At: https://www.guild.org.au/__data/assets/pdf_file/0016/13813/standard-pharmacy-vaccination.pdf
- SA Health. Organisations delivering immunisation programs. 2018. At: http://www.sahealth.sa.gov.au/wps/wcm/connect/b21c790047dce632bf2abf5c843e6e29/Organisations+delivering+immunisation+programs_Information+guide+and+application+form+V6.1+January+2018.pdf?MOD=AJPERES&CACHEID=ROOTWORKSPACE-b21c790047dce632bf2abf5c843e6e29-m1XbQ1T
- Northern Territory Government, Government Gazette. 16 March 2017. At: https://nt.gov.au/__data/assets/pdf_file/0011/405893/s9.pdf
- ACT Government Health. ACT Pharmacist Vaccination Standards. 2018. At: http://health.act.gov.au/sites/default/files//Pharmacist%20vaccinations%20-%20Standards_1.pdf
- Department of Health and Human Services, Tasmanian Vaccination Program Guidelines. 2016. At: https://www.dhhs.tas.gov.au/__data/assets/pdf_file/0020/211808/Tasmanian_Vaccination_Program_Guidelines_Feb_2016.pdf
- Healthy WA. Pharmacist Vaccination Code. 2018: At: http://www.healthywa.wa.gov.au/~/media/Files/Corporate/general%20documents/medicines%20and%20poisons/Word/Pharmacist_vaccination_code.ashx
- NSW Government Health. NSW Pharmacist Vaccination Standards. 2018. At: http://www.health.nsw.gov.au/pharmaceutical/Documents/pharmacist-vaccstandards.pdf
- https://www2.health.vic.gov.au/~/media/health/files/collections/policies%20and%20guidelines/v/victorian-pharmacist-administered-vaccination-guidelines%20-%20pdf.pdf
- https://www.guild.org.au/__data/assets/pdf_file/0016/13813/standardpharmacy-vaccination.pdf
- http://www.sahealth.sa.gov.au/wps/wcm/connect/b21c790047dce632bf2abf5c843e6e29/Organisations+delivering+immunisation+programs_Information+guide+and+application+form+V6.1+January+2018.pdf?MOD=AJPERES&CACHEID=ROOTWORKSPACE-b21c790047dce632bf2abf5c843e6e29-m1XbQ1T
- https://nt.gov.au/__data/assets/pdf_file/0011/405893/s9.pdf
- http://health.act.gov.au/sites/default/files//Pharmacist%20vaccinations%20-%20Standards_1.pdf
- https://www.dhhs.tas.gov.au/__data/assets/pdf_file/0020/211808/Tasmanian_Vaccination_Program_Guidelines_Feb_2016.pdf
- http://www.healthywa.wa.gov.au/~/media/Files/Corporate/general%20documents/medicines%20and%20poisons/Word/Pharmacist_vaccination_code.ashx
- http://www.health.nsw.gov.au/pharmaceutical/Documents/pharmacist-vacc-standards.pdf





 Adjunct Professor Manya Angley FPS (CredPharm MMR) Credentialed and Disability Pharmacist
Adjunct Professor Manya Angley FPS (CredPharm MMR) Credentialed and Disability Pharmacist Penny Beirne MPS
Penny Beirne MPS