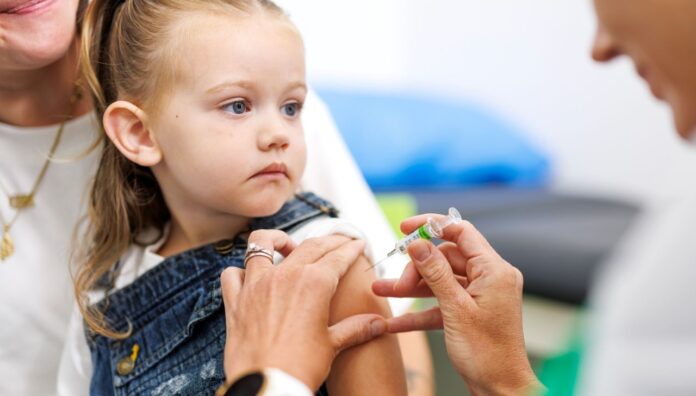
Busy pharmacies, bright lights and confined spaces can heighten fear surrounding vaccination, particularly among children who are neurodiverse.

Understanding how to create a safe, calm environment is essential to delivering patient-centred care.
A time sensitive vaccination window
With winter around the corner, pharmacies should be in peak winter vaccine campaign mode – including the recently introduced intranasal vaccine, FluMist.
But pharmacists new to vaccinating children are often nervous that immunising school-aged children can be tricky. The Child Health Poll reported that 1 in 4 children experience needlephobia – which often intensifies with age. These challenges are amplified amongst children who are neurodiverse, calling for an enhancement of personalised care throughout the vaccination process.
Yvette Anderson MPS – founder of Spectrum Pharmacist, which sets out to bridge the gap for neurodivergent families – told AP her top tips.
Fear surrounding the vaccination experience
Neurodiverse children can often experience heightened levels of sensory sensitivity, differences in communication, and increased anxiety in unfamiliar settings.
‘Early signs of anxiety and sensory overload vary from child to child,’ Ms Anderson said. ‘It is helpful to understand the child’s usual baseline before the appointment, because some behaviours may be part of their normal coping style rather than a sign of distress.’
During vaccination, early signs of overwhelm may include:
- increased fidgeting,
- tensing of the body
- changes in facial expression
- looking away
- covering ears
- becoming quieter
- repeating words
- asking the same question repeatedly
- becoming more restless or distressed.
Some children may also freeze, withdraw, resist touch, or become tearful or irritable.
In a health care environment, such as the pharmacy, environment sensory triggers may include:
- waiting for turn or appointment time (both pre- and post-vaccination)
- uncertainty surrounding the vaccination process, how it will feel being administered and who will be administering it
- bright lights, busy pharmacy environments, clutter and bright signage
- auditory considerations including loud phones ringing, loud conversations and/or multiple conversations, as well as sudden noises
- tactile considerations, including being touched, pressure on the site of injection, the smell and feel of alcohol wipes, and the needle prick or nasal spray itself
- Olfactory triggers including the smells in the pharmacy such as perfumes, disinfectants, other people
- Interoceptive, which can include perceived and actual pain, dizziness and perhaps fainting, heightened body awareness and anxiety.
Easing the process
Encouraging individuals to visit the pharmacy prior to the appointment ensures a sense of familiarity with the process and ease with the immuniser. Similarly, scheduling the appointment at quieter times during the day reduces sensory stimuli, which can be paired with devices such as iPads or music to make the process as smooth as possible.
Ms Anderson maps out a few reducing anxiety techniques, including:
- modifying the environment can reduce sensory overwhelm by up to 60%
- providing clear information (either written or visual) explaining the process for vaccination can reduce uncertainty
- empowering the individual to modify the environment to suit their needs
- having trained staff that utilise neuro-affirming practices
- engaging with Hidden Disabilities Sunflower Awareness
Changes and accommodations can range from a low sensory clinic, including a shorter waiting time or using topical lignocaine to to smooth over those processes.
‘The easiest thing that we can do as a profession is to ask what the needs of the patients are, and actively listen to concerns without judgement. Understanding the patient standing in front of you is probably the first and primary thing that we can do,’ Ms Anderson said.
‘Pharmacists can significantly reduce anxiety during vaccinations by using clear, direct language that prioritises predictability, choice, and calm pacing which avoids jargon, overly clinical terms, or vague reassurances.
‘Communication should be predictive and sequential, always stating what’s next, how long it takes, and what it feels like. Key language principles include keeping it short and literal with simple words, such as ‘pinch’ instead of ‘injection’ or ‘cool wipe’ instead of ‘antiseptic’ – limiting sentences to under 10–15 words.’
Pharmacists should communicate with parents before vaccination appointments using a warm, collaborative approach centered around trust and setting clear expectations.
This can be achieved by ‘Reaching out via phone, text or a short pre-appointment questionnaire a day or two ahead, framing it as a partnership, and inviting parents to describe behaviours, sensory triggers and preferred strategies’.
Ms Anderson stressed that ‘Referring patients to a GP should be a shared decision between the individual, their parent/guardian, and the pharmacist immuniser’.
‘If the pharmacist immuniser feels that it is out of their scope/training or confidence then ensuring the patient’s safety is imperative, which may include medical contraindications and consent complexities, which is a significant consideration in the neurodivergent population.’
Pharmacists can contact specialist immunisation services – available in each state and territory – that equip health professionals managing complex vaccination cases with advice and immunisation support.
These services can also facilitate referrals to adapted vaccination settings, such as low-sensory clinics or, where appropriate, sedation-supported pathways.
‘It is helpful to understand the child’s usual baseline before the appointment, because some behaviours may be part of their normal coping style rather than a sign of distress.’
Introduction of FluMist
The introduction of the intranasal alternative FluMist may be beneficial in reducing stress surrounding vaccination for neurodiverse children who have needlephobia.
As it is a novel approach, there may be an initial hesitation, Ms Anderson advised.
‘There might be a little bit of a barrier to start with, but I certainly think having that alternative is a really positive step forward.’
However, despite FluMust easing stress for individuals with needlephobia, it could be a sensory trigger to neurodivergent individuals who experience heightened sensory reactivity or sensory hyperarousal, she warned.
‘Being an intranasal vaccine, the process can involve brief pressure and tickling into the nasal passages, post-nasal drip, or an odd taste, and those sensations may be distressing for some, as the nose and throat are more likely to have a sensory reaction compared to the injection.’
Training opportunities
In collaboration with PSA, Ms Anderson is the founder of SpectrumRx, a foundational training program designed to help pharmacists, pharmacy assistants and students deliver the best possible care to neurodiverse people.
‘SpectrumRx provides complete neuro-affirming care for our pharmacy profession by providing education, awareness and understanding for all neurodevelopmental disorders,’ Ms Anderson said.
Through SpectrumRx , Ms Anderson emphasised the importance of creating social stories that clarify the details of the upcoming experience, which can be produced and given to families to provide an idea of what is to be expected – including in the vaccination process.
SpectrumRx will be launched at PSA26. Keen to come along? Register now!




 Diabetes medicines and peri-procedural blood glucose management
Diabetes medicines and peri-procedural blood glucose management
 Katie Phillips MPS[/caption]
Katie Phillips MPS[/caption]
 Erica Stephenson MPS with her kids[/caption]
Erica Stephenson MPS with her kids[/caption]
 Katie Phillip MPS with her two daughters[/caption]
Katie Phillip MPS with her two daughters[/caption]
 Deborah Hawthorne FPS with her two daughters[/caption]
Deborah Hawthorne FPS with her two daughters[/caption]


 Dr Amy Page (she/her) PhD, MClinPharm, GradDipBiostat, GradCertHProfEd, GradCertDMED, GAICD[/caption]
Dr Amy Page (she/her) PhD, MClinPharm, GradDipBiostat, GradCertHProfEd, GradCertDMED, GAICD[/caption]

 Amanda Quek (she/her) BPharm(Hons), GradCertAppPharmPrac[/caption]
Amanda Quek (she/her) BPharm(Hons), GradCertAppPharmPrac[/caption]


 ‘The Home of Pharmacists theme signifies belonging, connection, and purpose, uniting pharmacists across all areas of practice,’ said PSA National President Mark Naunton MPS.
‘The Home of Pharmacists theme signifies belonging, connection, and purpose, uniting pharmacists across all areas of practice,’ said PSA National President Mark Naunton MPS.