Residential aged care providers should be required to employ or retain at least one pharmacist as part of their allied healthcare team, according to the final report of the Royal Commission into Aged Care Quality and Safety.
Released on Monday (2 March), the 2,800-page report includes 148 recommendations from commissioners Tony Pagone and Lynelle Briggs to address what they describe as the ’poor quality … and fundamental systemic flaws with the way the Australian aged care system is designed and governed’.
It follows a 2-year investigation into the sector, including almost 100 days of hearings at which the commissioners heard from 641 witnesses, including residents, staff, families and experts.
Embedding pharmacists in residential aged care facilities (RACFs) was a central tenet in PSA’s submission to the royal commission in August last year.
‘It is essential that aged care facility residents and staff have regular and ready access to the expertise of pharmacists, even beyond the COVID-19 pandemic,’ the submission stated.
Other recommendations include improving access to timely and regular residential medication management reviews (RMMRs) and introducing stricter requirements for prescribing antipsychotic medicines to people in RACFs.
The PSA National President Associate Professor Chris Freeman said the report demonstrated how urgently the medicine safety problems in aged care need to be addressed.
‘Inappropriate chemical restraint, and polypharmacy leading to sedation, falls and avoidable hospitalisations are some of the biggest problems in aged care,’ he said.
‘Pharmacists are the key to solving these problems.’
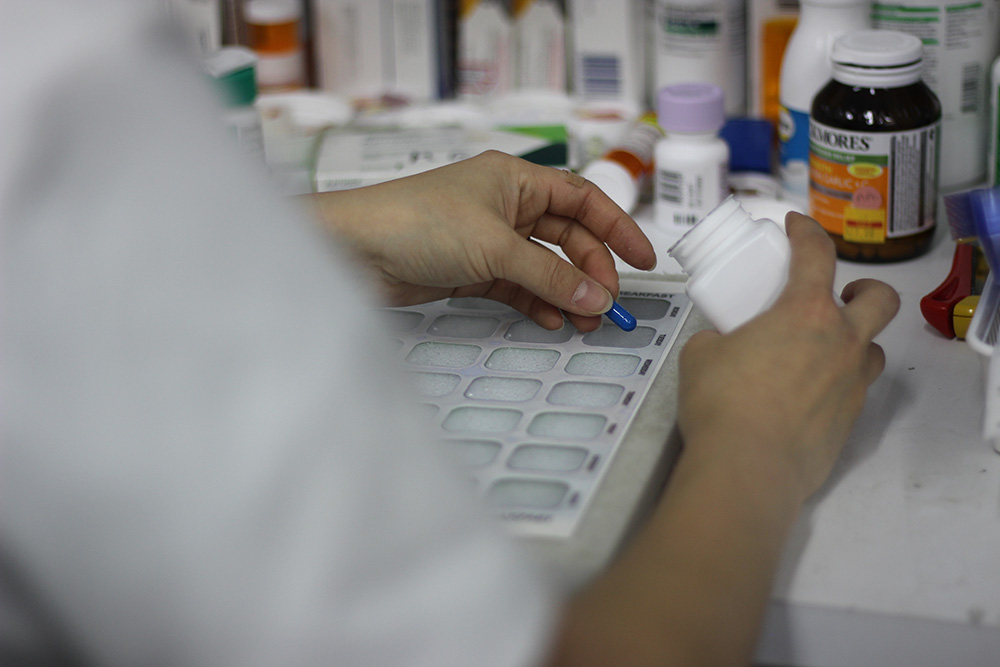 Improving medication reviews
Improving medication reviews
People living in RACFs are currently entitled to one RMMR every 24 months, unless there are significant changes to their medical condition or medicine regime.
The commissioners called on the federal government to ‘immediately improve access to quality medication management reviews for people receiving aged care’ by increasing access and funding for pharmacists to conduct RMMRs for every resident on entry to a facility, and annually thereafter, including respite care and transition care, by 1 January 2022.
‘With people living longer and the increasing prevalence of multi-morbidity, older people are more likely to be taking medicines and, in some cases, more likely to be taking multiple medicines daily,’ the commissioners wrote.
‘In aged care, medication management reviews are critical to reduce chemical restraints and other inappropriate use of medications.’
Reducing chemical restraint
The Royal Commission’s interim report, released in October 2019, identified the widespread use of chemical restraint in RACFs. In response, the government announced changes that were intended to address the issue.
‘These measures are commendable, but they do not go far enough to address a problem that has persisted for decades,’ the commissioners wrote in their final report.
Instead, the commissioners called on the government to introduce stricter requirements for prescribing antipsychotic medicines for people in RACFs.
They gave the example of risperidone, which is only subsided through the Pharmaceutical Benefits Scheme Schedule for the treatment of autism in children under the supervision of a paediatrician or psychiatrist.
‘We recommend a similar practice should apply to residential aged care: only a psychiatrist or a geriatrician should be able to initiate treatment with antipsychotic medicines for people in residential aged care,’ they wrote.
‘This will ensure that every person in residential aged care is reviewed by a specialist before antipsychotic medicines are begun.’
 Government response
Government response
Prime Minister Scott Morrison announced on Monday that the government would commit $450 million to address immediate issues raised in the report, followed by a more comprehensive response in the May budget.
He called the commission ‘the inquiry we needed to have’ and said the recommendations set out ‘a very important road map, which will establish generational change in this country when it comes to aged care’.
Other recommendations in the report include:
- enshrining the rights of older Australians in legislation, and providing universal entitlement for high-quality and safe care based on assessed need
- creating an independent inspector-general to investigate and monitor governance of the aged care system
- Implementing mandatory minimum qualifications for workers.
Minister for Health and Aged Care Greg Hunt said reform was necessary to respond to the ‘individual needs’ of older Australians.
‘We will put in place a new Aged Care Act … based on a simple concept of respect for the individual,’ he said.
‘Instead of being about providers, instead of it being about money, it’s about respect for the individual needs and that is the fundamental generational transformation.’
A/Prof Freeman said the recommendations in the report ‘challenge all of us to comprehensively rethink the way we support and protect older Australians’.
‘Putting in place quality indicators, improving clinical governance, increasing accountability, providing better staff training and ongoing professional development are all measures required if generational change to our aged care system is to be achieved,’ he said.
‘All of Australia’s 34,000 pharmacists have a critical role in improving medicine-related harm and providing a better aged care system and support for older Australians.
‘After 18 inquiries over 24 years, now is the time for action to improve the care for the Australians who need it the most.’
Read the final report from the Royal Commission into Aged Care Quality and Safety here.



 Yvette Anderson MPS[/caption]
Yvette Anderson MPS[/caption]


 Diabetes medicines and peri-procedural blood glucose management
Diabetes medicines and peri-procedural blood glucose management
 Katie Phillips MPS[/caption]
Katie Phillips MPS[/caption]
 Erica Stephenson MPS with her kids[/caption]
Erica Stephenson MPS with her kids[/caption]
 Katie Phillip MPS with her two daughters[/caption]
Katie Phillip MPS with her two daughters[/caption]
 Deborah Hawthorne FPS with her two daughters[/caption]
Deborah Hawthorne FPS with her two daughters[/caption]


 Dr Amy Page (she/her) PhD, MClinPharm, GradDipBiostat, GradCertHProfEd, GradCertDMED, GAICD[/caption]
Dr Amy Page (she/her) PhD, MClinPharm, GradDipBiostat, GradCertHProfEd, GradCertDMED, GAICD[/caption]

 Amanda Quek (she/her) BPharm(Hons), GradCertAppPharmPrac[/caption]
Amanda Quek (she/her) BPharm(Hons), GradCertAppPharmPrac[/caption]


 ‘The Home of Pharmacists theme signifies belonging, connection, and purpose, uniting pharmacists across all areas of practice,’ said PSA National President Mark Naunton MPS.
‘The Home of Pharmacists theme signifies belonging, connection, and purpose, uniting pharmacists across all areas of practice,’ said PSA National President Mark Naunton MPS.




