When it comes to person-centred care, bespoke tailoring to every patient’s healthcare needs is fundamental.
We all recognise that one-size- fits-all does not work when it comes to clothing. People have different needs from clothing in terms of protection, identity, size, shape, texture and impact.
Yet when it comes to providing health care, one-size-fits-all often prevails, presenting as a single care pathway for the ‘average patient’. This is a legacy of a biomedical model of care which optimises efficiency for health professionals and institutions, rather than patients.
What this results in is health services which are a poor or impossible fit for many people. The PSA National President Dr Fei Sim FPS says that two decades after patient-centred care was introduced, we still have a long way to go.
‘Patients should always be at the centre with all health professionals, including pharmacists, working together to provide seamless care,’ she says.
‘However, at a broader health systems level, the narrative needs to shift towards a person-centred model as opposed to a health professional-centred model.’
This sentiment is backed by evidence from numerous patients to the Royal Commission into Victoria’s Mental Health System (see boxed quotes throughout).
So what does person-centred care look like? According to PSA’s Clinical Governance Principles,1 ‘patient-centred care describes an approach to design and delivery of pharmacy services in which the service is genuinely built around the needs and preferences of consumers’, (see Figure 1). If achieved, it can make a big difference. There is a broad evidence base to support a person-centred approach to care, with outcomes including2;
- Improved patient satisfaction and engagement
- Lower mortality rates
- Reduced hospital readmission rates
- Reduced length of hospital stay
- Reduced healthcare acquired infections
- Improved adherence to treatment reduced healthcare costs.
The importance of person-centred care is shown in PSA’s recently revitalised Professional Practice Standards.3 It is one of three fundamental standards – along with ‘responsibility and accountability’ and ‘collaborative practice’ – that are ‘always relevant to all registered pharmacists, regardless of practice setting’.3 There are a number of influences on whether care is person-centred – including factors at an individual patient level, individual service level, health provider/organisation level and environment/system level.
The environment/system level relates largely to decisions and policies of those in regulatory or government departmental roles. At this level, a strong predictor of whether care is person- centered relates to the extent of listening and incorporating the perspectives of a wide breadth of individuals, their families and carers in system design. These influences are recognised to lead to more accessible, fit-for-purpose health policy decisions. An example of this is the extent of influence of patient support groups.
At a health provider/organisational level, person-centred care is improved through effective representation, consumer participation, quality improvement and facility design. The Australian Commission on Safety and Quality in Health Care has embedded these levers within its National Safety and Quality Health Service Standards,4 whic are applicable to all health services. While there are pockets of innovation, as a whole, service providers across the whole health system need more support to help health provider/organisational-level policies and decisions redesign care to be more person-centric. The Commission has developed guides, communities and networks to help institutions design more responsive and fit-for-purpose health care.
Thankfully, individual service and individual patient level progress can be easier to achieve. The skills and expertise of pharmacists can help provide individualised care through careful listening and responding to what is said. The prompts may sound like this: How well do you think your medicines are working for you? If you could get rid of one of your medicines, which would it be? Why is that?
To put all this into context, we spoke with some experts who provided case examples and insights.
The right environment
At a health provider/organisation level, the environment in which that health care is delivered is one of the most important aspects of person-centred care, says Dr Ramesh Walpola MPS, pharmacist, Pharmacy Academic Lead and Program Authority at the University of New South Wales’ School of Health Sciences.
In a recent study into patient experience, Dr Walpola and colleagues from Macquarie University and St Vincent’s Health Network found that feeling well treated, valued and comfortable had a significant impact on how a patient perceived a health service.5
‘The physical environment needs to be inviting for a patient,’ he says. ‘Do our patients feel comfortable talking here? Is it too noisy or too bright? Is there information available in a form they can understand?’ Other considerations include whether patients can easily navigate a pharmacy and find the items they need.0
‘The second element is the social environment we create within health care and whether our patients feel comfortable sharing themselves with us. While there has been a lot of work done by health professionals, managers and administrators to improve these elements, there is still a prevailing biomedical culture … And a need for health professionals and health services to be more holistic in their approach.’
While systemic change happens slowly, Dr Walpola says individual pharmacists can make improvements in primary care and community pharmacy settings.
He points to western Sydney’s Emerton Pharmacy, where husband and wife team Margaret Ruhnau MPS and Curtis Ruhnau MPS and their third partner Matthew Quick MPS have made simple changes to make their pharmacy a welcoming and safe environment for patients.
This includes looking into the Census data and the National Diabetes Services Scheme heatmap for their area to learn more about their community so as to tailor health literacy approaches to different groups. The ‘especially useful’ Census data, showed the cultural diversity of the area as well as a young population with low levels of completed education, Mr Ruhnau says.
Part of the environment also relates to cultural safety. His pharmacy team, many of whom wear hijabs, also speak Arabic, Mandarin, Urdu and Hindi.
The Census data also revealed a First Nations population surrounding the Emerton Pharmacy of between 6.8% and 15.3% (it is 3.4% nationally).
Connecting with community is key to improving their health, says MrRuhnau whose staff is involved with the Too Deadly for Diabetes program, has completed the Centre for Cultural Competency training course and is now working its way through PSA’s Deadly Pharmacist Foundation Training Course.
Communication and cultural competency are key
At an individual patient level, person- centred care can only happen when health professionals communicate effectively with people to fully understand their preferences and concerns.
‘We all know that pharmacists are great at taking a medication history and doing a medication review, but one area we could target to provide more person-centred care is acknowledging a patient’s narrative,’ says Megan DelDot MPS, clinical pharmacist and research assistant at the University of Queensland. This involves asking about a patient’s medicine experiences, expectations and preferences.
‘The pharmacist and patient can then agree on a person-centred medication plan that includes steps for ongoing monitoring and review,’ she says. ‘Demonstrating empathy and compassion can help patients feel more at ease discussing their feelings, worries and preferences about their health care, and can assist with building trusting relationships.’
Ms DelDot encourages pharmacists to proactively offer and create safe spaces for people to access the care pharmacists provide. She also identifies that some people – particularly people who have migrated from other countries – often prefer written information about medicines so they can go home, read about them and discuss them with their families.
Dr Walpola says pharmacists should seek out training about working with diverse populations to gain greater awareness and understanding.
‘It is important to develop your own self-awareness and reflection skills, so that you do not succumb to unconscious biases such as buying into stereotypes based on how a patient may present,’ he says.
A more connected system
Dr Ben Basger FPS is a clinical pharmacist at Wolper Jewish Hospital, a not-for-profit 55-bed facility in Sydney.
In an effort reduce the incidence of medicine problems following discharge, he implemented a discharge medicines review service with a more person-centred approach. In addition to typical aspects of medicine profiles at discharge, patients were actively encouraged to consult their GP and discuss specific recommendations that were important to them.
Prior to this approach, just 42% of GPs implemented Dr Basger’s recommendations. But following the new intervention strategy, which made the patient and/or caregiver the ‘driver of change’, 95% of patients took the recommendations to their GP, and three-quarters of these were acted upon.7
‘In hospitals, management has to believe in patient-centred care and be impressed by its importance,’ he said.
‘All pharmacists are capable of it with the right support.’
What matters
Health policy consultant Leanne Wells is the long-time former CEO of the Consumers Health Forum of Australia.
She tells AP: ‘There’s an adage that says rather than asking, “What’s the matter with you?” health professionals should instead ask, “What matters to you?
‘Person-centred care considers the full range of a patient’s needs and circumstances. This includes medical care and factors that affect health and wellbeing, such as loneliness and social isolation, lack of family support, unstable housing and food insecurity.’
Ms Wells points out that ‘unless clinicians appreciate factors that affect health beyond a treatment plan and understand a person’s motivations and capacity to self-manage, health outcomes may not be optimised, and a patient’s needs [may be] left unmet.’






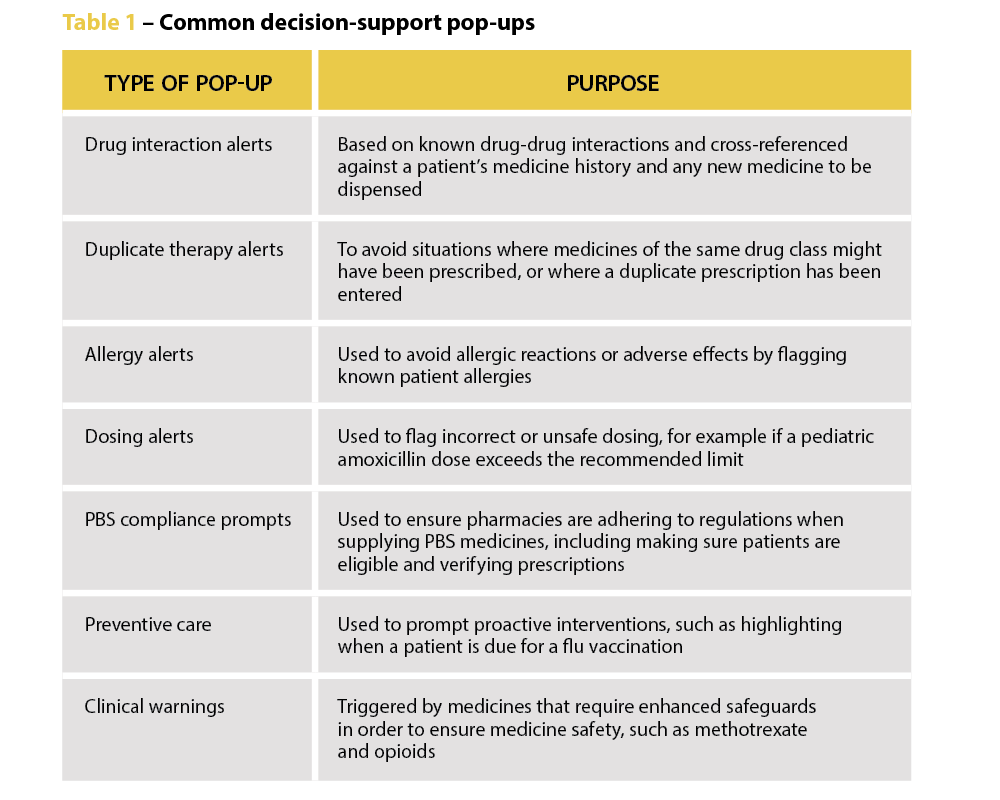 ‘We’re increasingly seeing incidents where alert fatigue has been identified as a contributing factor. It’s not that there wasn’t an alert in place, but that it was lost among the other alerts the clinician saw,’ Prof Baysari says.
‘We’re increasingly seeing incidents where alert fatigue has been identified as a contributing factor. It’s not that there wasn’t an alert in place, but that it was lost among the other alerts the clinician saw,’ Prof Baysari says.