
Homeless patients often have complex health needs and difficulty sticking to medicine regimens. Perth-based GP pharmacist Kate Fulford MPS uses her broad knowledge base to find the right approach.
As a student at the University of Western Australia, Ms Fulford was focused on a career in hospital pharmacy. But after securing a hospital internship post-graduation in 2016, she quickly realised it wasn’t her speed.
After working as a qualified pharmacist for less than a year, Ms Fulford left the hospital system to work as a consultant pharmacist for Dementia Training Australia in a role that comprised academia, writing education programs, developing apps and improving how residential aged care staff manage medicines in people living with dementia.
From there, she took part in PSA’s General Practice Pharmacist Program, using her dementia care and clinical pharmacist skills in a role at home aged care service Silver Chain, where she works as part of an integrated end-of-life care team.
‘[The PSA GP Pharmacist Program] opened up a lot of doors for me,’ Ms Fulford told Australian Pharmacist. ‘I’ve worked in four different practices now – some large, some small, all focused on developing a multidisciplinary team approach.’
Last year, she became the first pharmacist to join Street Doctor, a mobile health service for vulnerable people, including those living on the margins or experiencing homelessness, via PSA’s GP pharmacist pilot program.
While the role was initially funded through the WA Primary Health Alliance, Ms Fulford is now employed privately by Street Doctor after they saw the immense value of having a pharmacist on board.

Approaches that work: understanding each patient
Street Doctor‘s two mobile clinics are geared to function just like a normal GP clinic, complete with a multidisciplinary team of a GP, two nurses and a pharmacist.
After seeing the GP, patients move onto the nurse for a blood test, vaccinations or health assessment, followed by a consultation with Ms Fulford to discuss medicine issues and the barriers that may prevent them from taking their medicines correctly.
‘Then we all come together to discuss the case and raise the concerns we’ve noted, [which are] fed back to the GP who can immediately make changes based on our unique skill sets and knowledge.’
For the vulnerable homeless population, medicines are the most accessible health intervention. Street Doctor works closely with a few local community pharmacies who assist with supplying medications to those who can’t afford them.
‘It’s a very simple intervention, however this often means people are on a huge amount of medicines,’ Ms Fulford said. ‘They also bounce between healthcare systems and go into hospital more than most.’
Part of Ms Fulford’s role at Street Doctor is medicine reconciliation, which often entails analysing discharge summaries through My Health Record to figure out what medicines patients should be taking and corroborating this with their GP’s treatment goal.
Medicines reviews are also geared towards finding the best solution for the patient and their situation.
‘Adherence is a big issue and most of our patients can’t manage complicated medicine regimes,’ she said.
‘Adherence is a big issue and most of our patients can’t manage complicated medicine regimes.’
Best practice may indicate a medicine should be taken twice daily or on an empty stomach, but these conditions are often not possible among the cohort of patients.
‘[We] change things to suit the person and work with them to figure out what they can manage and how they feel the treatment plan will work for them.’
Improving prescribing
Having a pharmacist on the team helps to improve both prescribing practices and patient outcomes.
‘Now that I’ve been there for so long, patients trust me and know that I’m not going to push something onto them that they don’t want to do,’ Ms Fulford said.
GPs can also develop treatment plans much faster with Ms Fulford’s input. She helps to get the patients on board through motivational interviewing, taking time off the GPs’ hands so they can see more patients.
As a former hospital pharmacist, Ms Fulford knows how the healthcare system works and where to source information, along with the challenges that can be encountered upon discharge when updated medicine lists don’t go through to a community pharmacy.
One recently discharged patient, a woman in her 60s who was in intensive care due to medicine induced euglycemic diabetic ketoacidosis, had substantial changes made to her medicines during her long hospital stay.

But when that information was not relayed to the community pharmacist, she inadvertently went back onto the same medicines that led to her hospitalisation in the first place.
‘She didn’t have the capacity to recognise that what she was currently taking was not what the hospital had intended, and she wasn’t put back on her insulin when she was supposed to be,’ Ms Fulford said.
After a consultation with the patient 2 days post-discharge, she quickly picked up on the problem.
‘With the help of her community pharmacy, we got the changes made that day and quickly linked her in with Silver Chain to administer her insulin [along with] teaching her how to [inject] insulin and check her blood sugars,’ she said.
Providing specialist care
Diabetes is a health condition often encountered at Street Doctor, due to the high number of Aboriginal and Torres Strait Islander patients and the difficulty homeless people can face accessing quality food.
While an endocrinologist runs the diabetes clinic, before Ms Fulford arrived there was a large gap in medicine education and patient follow-up. This is vital to ensure patients understand changes to their medicine and how to manage their new insulin, sick day management or correcting low blood sugar.
To ensure the changes stick, Ms Fulford makes it clear to patients that she’s available for multiple consultations, whether for mental health counselling or lessons in using a glucometer.
In terms of medicines optimisation, Ms Fulford often steers GPs and specialists away from their go-to medicines to another option that works better from an adverse effects profile.
Each specialist is focused on managing a singular condition, but Ms Fulford brings a multimorbidity perspective to medicines.
The psychiatrist at the clinic, for example, often prescribes medicines which may cause adverse effects such as weight gain or sexual dysfunction.
This was the case recently, when a patient in his 30s who had suffered a heart attack was prescribed mirtazapine to alleviate his anxiety and insomnia, which were the two biggest complaints he expressed in the psychiatric consultation.
Knowing the patient has diabetes, several cardiac risk factors and has struggled to reduce his weight, Ms Fulford realised the medicine wasn’t a good fit.
She addressed this with the psychiatrist, suggesting they switch to a medicine that doesn’t cause weight gain and can be taken in the morning, due to the patient’s known night-time nonadherence.
‘It’s about changing things to suit the person and working with them to figure out what they can manage and how they feel the treatment plan will work for them.’
‘We swapped him to an SSRI [Selective serotonin reuptake inhibitor] in the morning,’ Ms Fulford said. ‘And he has continued losing weight, his diabetes is [under] control and his mental health is improving, just by choosing the right medicine.’
Because Ms Fulford was present during the consultation, she was able to make the relevant changes before the patient left the consult and faced a failed treatment outcome.
‘Treatment failure really affects their trust in the healthcare system and their willingness to try something the next time, because they’ve had this bad experience,’ she added.
A doctor’s perspective
From a GP point of view, having Ms Fulford on the Street Doctor team is a huge advantage.
‘She’s a wealth of knowledge,’ Dr Priya Krishnan told AP. ‘She keeps up to date on all the current guidelines and she knows when various medicines might no longer be applicable, are out of date or have been recalled.’
Dr Krishnan said Ms Fulford’s expertise extends far beyond medicines, including intricate knowledge of immunisations, assisting in health assessments, documentation for care plans and helping patients through addiction.
Ms Fulford also takes the time to talk through patient concerns, for example addressing vaccine hesitancy which will help to increase uptake of the COVID-19 vaccine among Street Doctor’s patients.
‘As GPs, because we’ve got a massive line of people waiting outside the caravan, it’s really hard to spend that time [talking] to them,’ Dr Krishnan said. ‘So I often just say, go and speak to Kate, she’s going to explain it to you.’
Patent education is another of Ms Fulford’s fortes.
‘Managing diabetes is huge, and she’s wonderful with that because she can explain to the patient why their medicines might have changed or certain adverse effects to be expected,’ Dr Krishnan added.
Before Ms Fulford joined the team, Ms Krishnan would usually have to call a local community pharmacist for advice.
‘But because Kate knows our patients’ histories, their family situations and financial position, she’s really good at being more comprehensive.’




 Adjunct Professor Manya Angley FPS (CredPharm MMR) Credentialed and Disability Pharmacist
Adjunct Professor Manya Angley FPS (CredPharm MMR) Credentialed and Disability Pharmacist Penny Beirne MPS
Penny Beirne MPS



 This CPD activity is sponsored by Reckitt. All content is the true, accurate and independent opinion of the speakers and the views expressed are entirely their own.[/caption]
This CPD activity is sponsored by Reckitt. All content is the true, accurate and independent opinion of the speakers and the views expressed are entirely their own.[/caption]
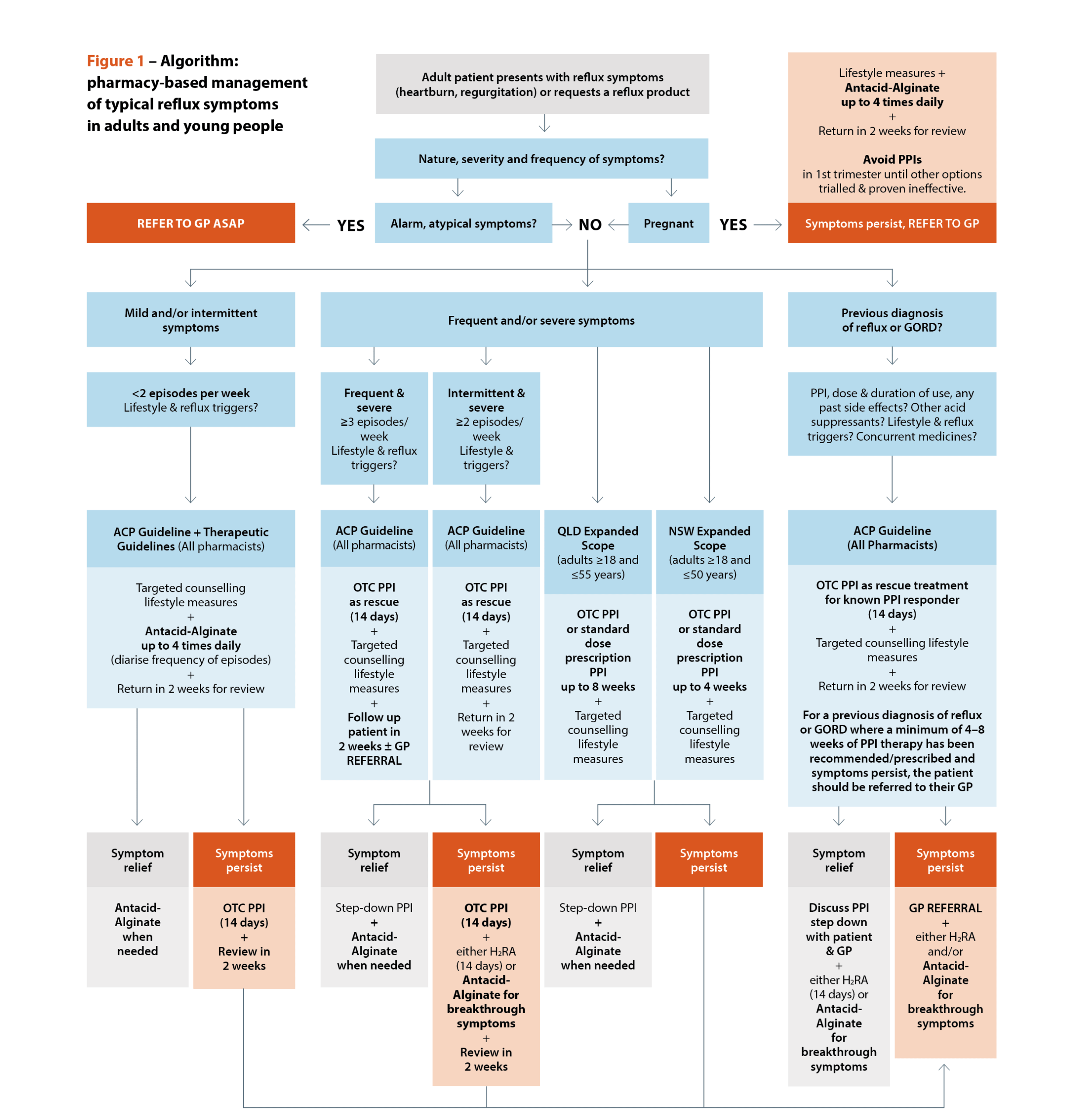 Sources: Australasian College of Pharmacy. Management of reflux: a guideline for pharmacists. Queensland Health. Queensland Community Pharmacy Gastro-oesophageal Reflux and Gastro-oesophageal Reflux Disease – Clinical Practice Guideline. NSW Health. NSW Pharmacist Practice Standards for gastro-oesophageal reflux and gastro-oesophageal reflux disease.[/caption]
Sources: Australasian College of Pharmacy. Management of reflux: a guideline for pharmacists. Queensland Health. Queensland Community Pharmacy Gastro-oesophageal Reflux and Gastro-oesophageal Reflux Disease – Clinical Practice Guideline. NSW Health. NSW Pharmacist Practice Standards for gastro-oesophageal reflux and gastro-oesophageal reflux disease.[/caption]





