A new National Core Community Palliative Care Medicines List highlights the medicines community pharmacies should keep in stock to support patients at the end of life.
In the final stages of life, symptoms like pain, breathlessness and nausea can escalate quickly. When that happens, families and clinicians often need medicines urgently to keep a patient comfortable.
Access to those medicines can also determine where someone spends their final days. Around 70% of Australians would prefer to die at home, but only a small minority are able to do so.
To support timely management of end-of-life symptoms, Palliative Care Australia, in collaboration with the PSA, Ageing Australia and Caring@Home, have developed a National Core Community Palliative Care Medicines List – identifying four medicines commonly required in the terminal phase of illness.

What’s on the list?
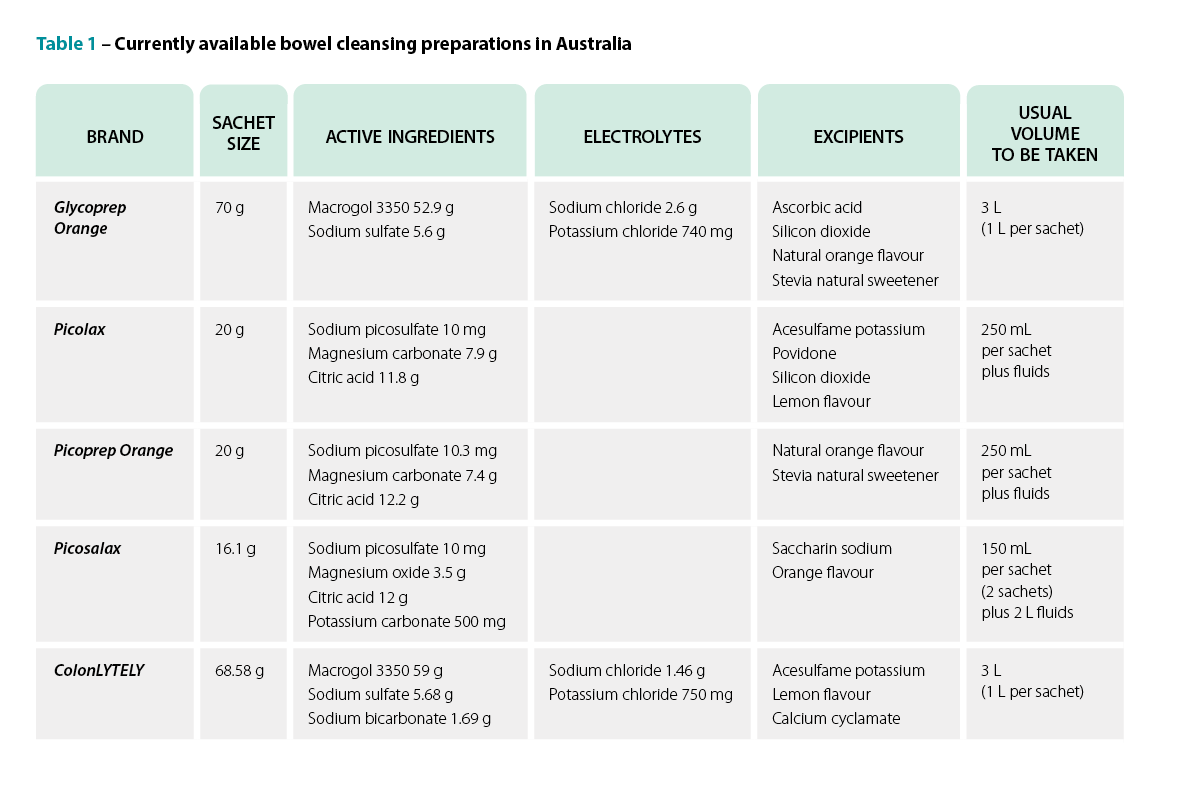
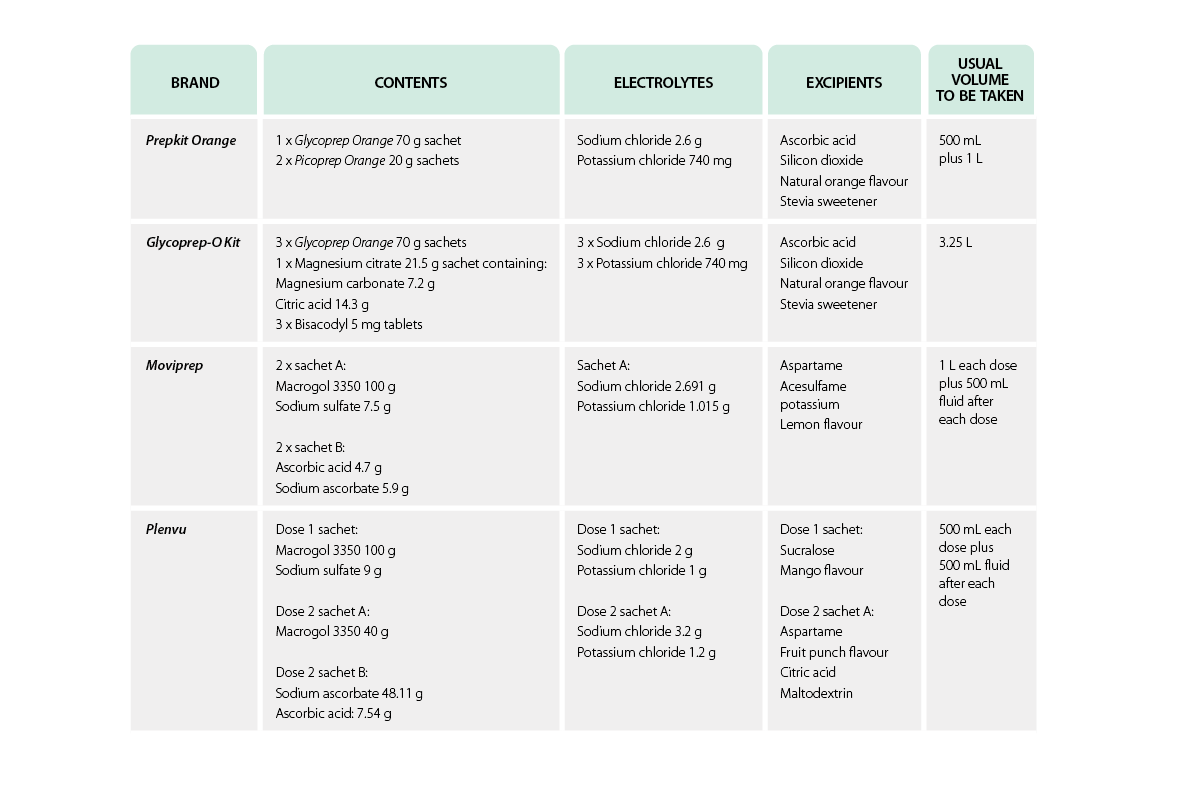
The medicines on the core palliative care medicines list include:
- clonazepam
- haloperidol
- hyoscine butylbromide
- morphine
All four medicines are available in formulations other than tablets, including oral drops and injectable forms, allowing for administration when swallowing becomes difficult.
Pharmacists are advised to stock the medicines on the list to allow for rapid dispensing. These medicines are often needed with little warning, said Tanya Maloney MPS, pharmacist and owner of TerryWhite Chemmart Coffs Harbour.
‘Medication can change quite quickly in those last few days,’ said Ms Maloney. ‘And there are a few ways we can help. We can talk to patients about anticipatory prescribing and encourage them to talk to their prescriber about getting those medications on hand so that when they need them, it’s not in the middle of the night when nothing’s open.’
TerryWhite Chemmart Coffs Harbour has committed to keeping the four core medicines in stock, and offers to arrange delivery so patients and carers do not have to travel between pharmacies to find them.
‘If we can take those friction points out of the equation for them and make everything easier and less stressful, that is where our role can really come in,’ she said.
Making palliative care support easier to find
Australia’s population is rapidly ageing, with the demand for palliative care estimated to double by 2035. Ms Maloney has seen this shift firsthand.
‘Around 2021, one of our regular patients became palliative, and one of our staff members had a mum who became palliative around the same time,’ she said.
‘Back then, we weren’t confident in asking those questions or having those conversations. But [supporting] these two particular patients and finding out what a different experience we could create by acknowledging what they’re going through and being part of that journey opened our eyes to [the fact that] we can really play an important role here.’
Since then, Ms Maloney and her team have worked to strengthen the pharmacy’s role in supporting palliative care patients in their community.
And as her team became more involved in this space, she identified that pharmacy support was not always as visible or integrated into the care pathways as other services.
‘[Many] services seem to work seamlessly for the patient – all these health practitioners will just turn up at your door to give you their support and services. But when it comes to prescriptions for pharmacies there was this real gap where patients and carers were still on their own and having to navigate that themselves.’
In response, Ms Maloney and her team looked for ways to become more involved and visible in the care network.
‘We’ve made that connection with our local palliative care team by letting them know that we’re there to help, that we’re keeping those medications in stock, and that their patients can let us know if they need home deliveries,’ she said.
Ms Maloney’s pharmacy is also listed on HealthDirect’s Service Offering in the pharmacy directory for ‘Palliative care medicine’ – pharmacies that stock medicines from the National Core Community Palliative Care Medicines List can activate this Service Offering, allowing patients as well as clinicians to see which pharmacies stock these medicines in the local area.
‘The more we can let people know what we do, the better, because it’s something people often might not want to talk about,’ she said. ‘Healthdirect is a no-brainer – it’s there for that reason. It’s getting out there what services you offer and making it easy for people to connect with you.’
Supporting patients and families at the end of life
Once patients begin receiving end-of-life care at home, pharmacies may also play a role in helping carers manage changing medication needs.
‘We can take the time to do a medication review of what they’re currently on, and just look at what we can do to simplify it,’ Ms Maloney said. ‘That might be suggesting deprescribing certain [medicines] that they don’t need anymore, so we can focus on the medications that are important at the time.’
‘We can talk to patients about anticipatory prescribing and encourage them to talk to their prescriber about getting those medications on hand so that when they need them, it’s not in the middle of the night when nothing’s open.’
Tanya Maloney MPS
Pharmacies can also help reduce practical burdens for carers who may already be managing complex responsibilities at home.
‘We often offer to set up an account for them so we can just put things on there and deliver them,’ she said. ‘We also let them know that after the person has passed, we can go and pick up the medications that they no longer need and safely dispose of them.’
In order for these supports to be effective, pharmacists need to feel comfortable opening conversations about what patients and families are experiencing.
‘Be prepared to get a bit out of your comfort zone,’ Ms Maloney said. ‘Just jump in and start trying to have those difficult conversations. And the more you do it, the easier it gets.’
Watch this short video to see how to update your pharmacies listing on the National Services Health Directory for Palliative Care.





 Yvette Anderson MPS[/caption]
Yvette Anderson MPS[/caption]