The Pharmaceutical Benefits Advisory Committee (PBAC) recently recommended the inclusion of additional medicines to ongoing arrangements for Continued Dispensing, after considering stakeholder feedback from consumer, medical and pharmacy organisations.
These come into effect as the much broader temporary Continued Dispensing emergency measure ceases at the end of June 2022.
Here is a run down of the most significant changes that impact pharmacists, which will come into effect on Friday (1 July).
1. Antidepressants and antiepileptic medicines are gone, as most PBS medicines fall off the list
Out of the 906 medicines listed in Pharmaceutical Benefits Scheme (June 2021), only 168 will be accessible through the expanded ongoing PBS Continued Dispensing arrangements.
Medicines to manage chronic diseases such as asthma, diabetes, and heart disease, have been prioritised, as well as medicines to treat HIV.
But not all stable chronic conditions are represented. Conditions such as depression or epilepsy have been overlooked, along with some medicines to treat chronic obstructive pulmonary disease such as tiotropium (Spiriva).
A huge range of medicines will no longer be able to be supplied under this PBS measure, such as medicines for migraines, anti-infective agents and pain medicines.
Other medicines of note that are absent include amiodarone, proton pump inhibitors such as omeprazole, esomeprazole and pantoprazole, and digoxin.
While far better than the situation in 2020, the regression to a limited formulary of medicines available through Continued Dispensing is disappointing, said incoming PSA National President Dr Fei Sim.
‘During the pandemic, pharmacists demonstrated nation-wide, on a large scale, that essential medicines can be safely and effectively provided to Australians in a timely manner through Continued Dispensing. There were no negative outcomes observed from the full program over the past 2 years – demonstrating sustained evidence,’ she said.
This decision reduces patient access to medicines at a time when they need it the most, Dr Sim warned.
‘The benefits of continuing the full scope of PBS Continued Dispensing as it was through the emergency measure outweigh any potential risks,’ she said. ‘The PSA will continue strong advocacy efforts to enable timely access to medicines [for] all Australians, because we all deserve better access to healthcare.’
2. The new PBS measures are permanent
When Continued Dispensing was introduced in 2012, only statins and oral contraceptives were accessible through the arrangements.
Continued Dispensing temporarily expanded to all PBS medicines in January 2020, following the bushfires and the start of the COVID-19 pandemic.
Now, the shorter list of available PBS medicines is here to stay. But there is a new requirement to ensure access to these medicines through Continued Dispensing: the patient’s doctor must be uncontactable and/or unable to provide a prescription.
3. Can I process Continued Dispensing as private supply (non-PBS)? Depends where you practise.
Medicines that are not on the new PBS list can be supplied as non-PBS Continued Dispensing medicines in states that have extended their current emergency orders.
Victoria issued a 6-month extension to Public Health Emergency Order No. 2, which will now expire in December 2022. New South Wales extended emergency orders by 3 months, expiring in September, under Section 10(4)(d) of the Poisons and Therapeutic Goods Act.
The PSA understands most states will automatically adopt the Commonwealth PBS changes. But it is not yet clear the regulatory mechanisms that will be used to achieve this or how this will affect non-PBS medicines.
The varying rules mean pharmacists could supply an antidepressant such as fluoxetine as a non-PBS Continued Dispensing medicine in NSW and Victoria, but not another state, for example.
Supplying relatively low-cost medicines such as fluoxetine through emergency orders might not be too costly for most patients. But it will be prohibitive in some cases.
Accessing high-cost medicines via non-PBS Continued Dispensing arrangements could leave patients hundreds or thousands of dollars out of pocket when they normally pay between $6.80 and $42.50 under the PBS, effectively cutting off access to essential medicines in an emergency.
Dr Sim said PSA is committed to supporting pharmacists through these changes.
‘As further information becomes clear, PSA will communicate these changes to members, including via PSA’s industry leading COVID-19 Regulatory Changes microsite,’ she said.
4. The ‘previous supply’ window will narrow to 3 months
Medicines can currently be supplied through Continued Dispensing if provided within a 6-month period. But under the new arrangements, Services Australia will reject Continued Dispensing if there is no record of supply of the medicine in the previous 3 months.
This might prove problematic for medicines such as thyroxine, which has up to 200 doses per box, or medicines with variable doses such as insulin.
5. Closing the Gap initiative will finally be recognised
The Closing the Gap PBS Co-payment Program, which reduces or removes the PBS co-payment for eligible Aboriginal and Torres Strait Islander people, will apply to medicines supplied under Continued Dispensing from 1 July. This initiative addresses an access equity issue that has always existed for Continued Dispensing.
Important fast facts for pharmacists
- Continued Dispensing will still only be accessible once per year.
- Pharmacists still need to determine if a medicine has been used through Continued Dispensing arrangements via dispensary history or My Health Record, a labelled box, or a phone call to another pharmacy.
- Where applicable, PBS Authority items can be issued under Continued Dispensing arrangements, but not in increased quantities. If a patient is usually supplied 2 x 30 packs of atenolol on PBS Authority, for example, only one pack can be supplied under Continued Dispensing.






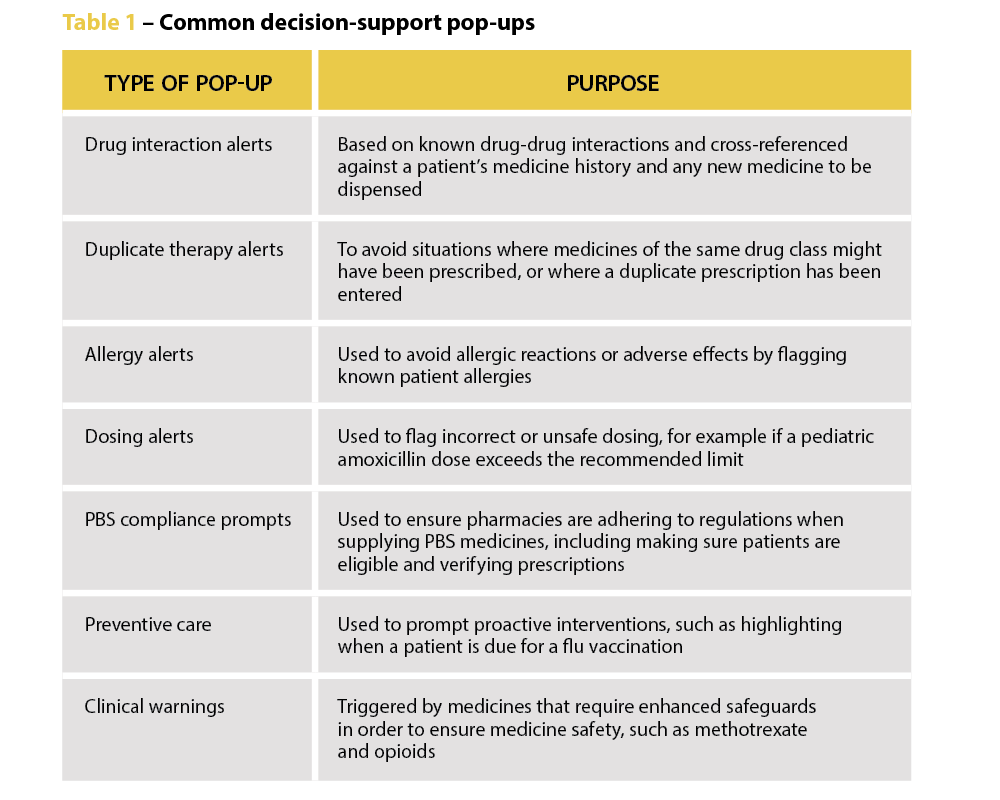 ‘We’re increasingly seeing incidents where alert fatigue has been identified as a contributing factor. It’s not that there wasn’t an alert in place, but that it was lost among the other alerts the clinician saw,’ Prof Baysari says.
‘We’re increasingly seeing incidents where alert fatigue has been identified as a contributing factor. It’s not that there wasn’t an alert in place, but that it was lost among the other alerts the clinician saw,’ Prof Baysari says.